Cataract Surgery in Glasgow, Kentucky

Glasgow Cataract Surgery Centers
After a lifetime of clear vision, one day it can seem as if your vision is failing and even a new eyeglass prescription can’t help. You might have cataracts, but don’t panic! There’s still hope. You can see life clearly again without cataracts with the help of our expert eye doctors at McPeak Vision Partners in Glasgow, KY. We offer cataract surgery treatment using state-of-the-art technology and techniques to reclaim your vision.
Escape the fear and frustration of cataracts and book an appointment today!
What Are Cataracts?
A cataract is a clouding of the lens inside your eye. Think of the lens like a window: when it becomes cloudy, it’s more difficult to see through the window clearly. Cataracts affect the eye in much the same way. Cataracts are a natural part of the aging process. Everyone begins to develop cataracts around age 50 and symptoms worsen in a large number of people. More than half of all Americans will have cataract surgery by age 80. When a cataract forms, clouding prevents some of the light from passing through the lens, resulting in poor vision.
What Causes Cataracts?
Cataracts are most often the result of the natural aging process, as proteins in the lens of your eye break down and clump together. This usually starts around age 40, and may not be noticeable until around age 60, but can vary from person to person. It is widely believed that exposure to ultraviolet light also contributes to the growth of cataracts. Although less common, cataracts can be congenital, the result of another disease in the body, or develop after an eye injury.
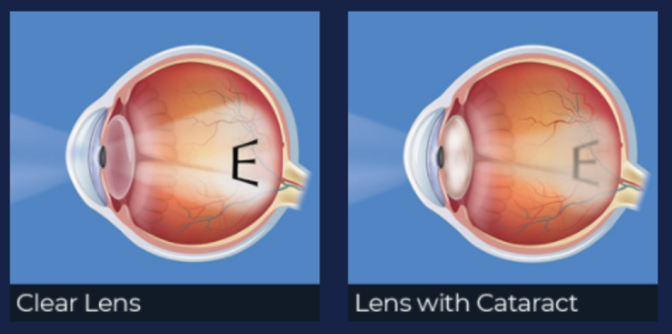
For most people, cataracts progress slowly. Eventually, cataracts can impair your vision and impact your daily activities, requiring surgical treatment.
Fortunately, the cloudy natural lens in your eye can be safely removed and replaced with a man-made lens with specific focusing power for your individual needs.
To find out if you qualify for cataract surgery, call the experienced Glasgow eye surgeons of McPeak Vision Partners and book a consultation today.
Symptoms of Cataracts
If you’re experiencing any of the following symptoms, you may have cataracts, and could potentially benefit from life-changing cataract surgery:

Cloudy or blurred vision

Double vision

Faded colors

Trouble seeing at night

Light and glare sensitivity

Seeing halos around lights
If you have any of these symptoms or have been told you have cataracts, request an appointment online, or call 270-781-4909 to schedule an evaluation with the cataract surgeons of McPeak Vision Partners today.
Cataract Removal & Treatment
When cataracts begin to impair your quality of life, it is important to have an evaluation with your eye doctor. You can take advantage of a once-in-a-lifetime opportunity to achieve better vision—potentially even better than you had before cataracts developed.
Cataract surgery is one of the most commonly performed procedures in the U.S. It’s a brief painless outpatient procedure during which the eye’s natural lens is removed and replaced with an intraocular lens (or IOL for short). Cataract removal and lens implantation are safe and effective. At McPeak Vision Partners, we are pleased to offer a variety of Advanced Technology Intraocular Lens (ATIOL) options to our patients.
Advanced Technology Intraocular Lenses (ATIOLs)
Patients who wish to further improve their vision can do so with ATIOLs. The best lens for you depends on many factors, including your lifestyle and specific vision needs. In addition to removing the symptoms of cataracts, these advanced lenses can also correct nearsightedness, farsightedness, astigmatism, and even age-related loss of near vision (presbyopia). ATIOLs can help reduce or even eliminate the need for eyeglasses and contacts. Additional costs are involved, and many patients choose to use an interest-free financing option or pay with cash or credit card. Contact us to discuss your options.
Basic Monofocal (Single-Focus) IOLs
If you don’t mind wearing glasses, you may opt for a basic monofocal (single-focus) IOL. This traditional lens is used to replace the cloudy lens of the eye, reversing the effects of cataracts. This technology has been available for many years and improved millions of patients’ vision. The lenses correct your vision for one distance only. This means that you will continue to be dependent on glasses for some tasks, such as reading. Basic monofocal IOLs are covered by most medical insurance plans.
Our Glasgow, KY cataract surgeons at McPeak Vision Partners use the most advanced lenses and will be happy to discuss the best option for your unique eyes. Schedule a consultation with a McPeak Vision Partners cataract eye surgeon today to find out which intraocular lens option is the best fit for you.
Laser Cataract Surgery in Glasgow
McPeak Vision Partners is proud to be leaders in laser cataract surgery for the Glasgow, Kentucky area. Laser cataract surgery eliminates the need for a surgical blade and offers our patients an incredibly precise procedure with optimized results.

Schedule Your Cataract Surgery Consultation at McPeak Vision Partners
Looking to have cataract surgery in or around Glasgow, KY? Find a McPeak Vision Partners location near you!
Call or click to book an appointment at either our Bowling Green or Glasgow, Kentucky locations to learn if you qualify for cataract surgery.
Frequently Asked Questions About Cataracts
There is no certain way to prevent the development of cataracts or to slow their progression. However, taking the following steps to safeguard the health of your eyes may help:
Undergo regular eye examinations
Eat a healthy diet
Don’t smoke
Wear sunglasses with UV protection
Address other health problems
Cataracts are a natural part of the eye’s aging process and impact everyone. However, there are some risk factors that may put certain people at higher risk for developing cataracts at an earlier age. These include:
Diabetes
High blood pressure
Nearsightedness
Obesity
Smoking
Excessive sunlight exposure
Previous eye surgery
Eye injury and/or inflammation
Use of corticosteroid medications
Excessive alcohol consumption
Yes. If you’ve had LASIK surgery in the past you can still have cataract surgery.
When cataracts progress to the point where clouding of the lens causes vision loss or impairment that impedes daily activities, cataract surgery is deemed medically necessary and is typically covered by medical insurance.
Basic Intraocular Lenses (IOLs) will eliminate the cloudiness caused by cataracts and are covered by insurance, but you may incur out-of-pocket expenses if you and your surgeon choose an advanced technology implant (ATIOL) or laser technology.
Be sure to ask your surgical counselor about flexible payment options.
No, each eye is operated on separately, usually 1-4 weeks apart.
Eye surgery is like surgery on any other body part—there will be a period of recovery. Fortunately for cataract surgery, this time is minimal. Your vision will be blurry right after surgery, but most patients are able to go back to normal daily activities in as little as 24-48 hours.
While you are awake during cataract surgery, your doctor will use anesthetic eye drops to numb your eyes. You will also be given a sedative to help you relax during the procedure.
The actual procedure is not painful. Most patients feel mild to moderate irritation for the first few days after surgery, similar to having an eyelash in the eye. Artificial tears may be used as often as necessary to reduce this irritation.
ATIOLs (Multifocal implants for astigmatism and presbyopia) may help you avoid having to wear glasses or contacts altogether. Using a basic single-focus implant, you will still require at least a reading prescription. Be sure to ask your doctor about your advanced technology implant (ATIOL) options.
Once removed, cataracts cannot return. In some cases, however, cloudiness (posterior capsule fibrosis) may occur in the lens capsule months or years after surgery. This eye condition is also treatable with a safe and painless laser procedure.
Our McPeak Vision Partners eye care centers in Kentucky
McPeak Vision Partners has two convenient locations in Kentucky as well as a surgery center. Our skilled Bowling Green and Glasgow eye doctors look forward to providing excellent eye care in the communities they continue to serve. Schedule your comprehensive eye exam, LASIK consultation, or shop for your new favorite frames! Learn more.
“More than half of all Americans will have cataract surgery by age 80.”
Reference: 1. Facts about cataract. National Eye Institute Website. https://nei.nih.gov/health/cataract/cataract_facts. Accessed March 08, 2022.

 270-781-4909
270-781-4909 270-843-9678
270-843-9678